Acute Limb Ischemia (ALI) is a sudden decrease in blood flow to a limb, threatening its viability and requiring immediate medical attention. Timely diagnosis is critical, as delays can lead to irreversible tissue damage, limb loss, or even death. We will explores the diagnostic approaches, essential investigations, and clinical strategies for detecting ALI effectively.
Understanding Acute Limb Ischemia
Acute Limb Ischemia occurs when arterial blood flow to an extremity is abruptly reduced, usually due to thromboembolism, arterial thrombosis, or trauma. ALI commonly affects the lower limbs but may also involve the upper limbs. Typical risk factors include atrial fibrillation, peripheral artery disease (PAD), recent surgery, or hypercoagulable conditions.
Clinically, ALI presents with the “6 Ps”
- Pain: Sudden and severe.
- Pallor: Pale or mottled skin.
- Pulselessness: Absence of distal pulses.
- Paresthesia: Numbness or tingling sensation.
- Paralysis: Muscle weakness indicating advanced ischemia.
- Poikilothermia: Cold limb due to lack of blood flow.
Recognizing these symptoms early is key to prompt diagnosis and intervention.
Diagnosis of Acute Limb Ischemia
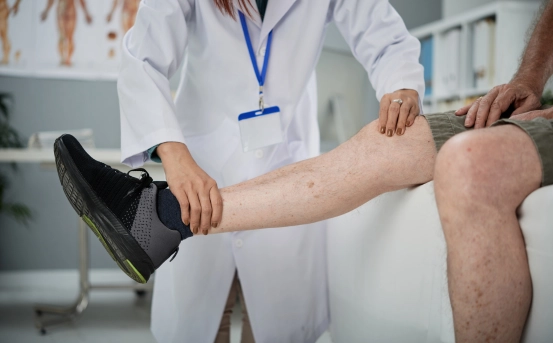
The first step in diagnosing ALI is a thorough clinical evaluation. A detailed medical history should focus on cardiovascular risk factors, recent interventions, or embolic sources such as atrial fibrillation. Physical examination should include
- Palpation of pulses in the affected and contralateral limb.
- Assessment of capillary refill and skin temperature.
- Neurological evaluation to detect sensory or motor deficits.
Clinical scoring systems like the Rutherford classification help categorize the severity of ALI and guide urgent management decisions.
Laboratory Investigations
Although ALI is primarily diagnosed clinically, laboratory tests support the overall assessment and help identify underlying causes. Key investigations include
- Complete Blood Count (CBC): Detects infection, anemia, or thrombocytosis.
- Coagulation Profile: PT, aPTT, INR to evaluate clotting disorders.
- Renal Function Tests: Creatinine and blood urea nitrogen (BUN) to assess kidney function before contrast imaging.
- Cardiac Enzymes: In cases of embolic sources from myocardial infarction.
- D-dimer Test: Elevated levels can indicate thrombotic events but are non-specific.
These investigations are especially useful when ALI is secondary to systemic conditions.
Imaging Modalities for Diagnosis
Imaging is essential to confirm the diagnosis, locate the obstruction, and plan therapeutic intervention. Commonly used modalities include
- Duplex Ultrasonography :- Duplex ultrasound is a first-line, non-invasive imaging technique that combines B-mode imaging and Doppler flow assessment. It helps detect arterial occlusion, stenosis, and blood flow dynamics. Advantages include bedside availability and no radiation exposure, making it suitable for unstable patients.
- Computed Tomography Angiography (CTA) :- CTA provides detailed, high-resolution images of the arterial system and helps identify thrombi, emboli, or arterial dissection. CTA is fast and widely available, though it requires contrast administration and careful evaluation of renal function.
- Magnetic Resonance Angiography (MRA) :- MRA is useful in patients with contrast allergies or renal insufficiency. It provides precise vascular mapping and can evaluate collateral circulation. Limitations include cost, availability, and longer scan times.
- Conventional Digital Subtraction Angiography (DSA) :- DSA remains the gold standard for definitive diagnosis and simultaneously allows endovascular intervention. It provides detailed visualization of the arterial tree, enabling precise localization of blockages and planning for thrombolysis or surgical embolectomy.
Differential Diagnosis
Several conditions mimic ALI, and differentiating them is critical to avoid unnecessary interventions. Common differentials include
- Chronic Limb Ischemia: Usually has gradual onset, collateral circulation, and less severe pain.
- Compartment Syndrome: Pain with swelling, tense compartments, and neurologic deficits.
- Peripheral Neuropathy: Chronic numbness or tingling without acute ischemic changes.
- Deep Vein Thrombosis (DVT): Usually presents with limb swelling, redness, and tenderness, not pulselessness.
Accurate differentiation ensures appropriate treatment and prevents complications.
Multidisciplinary Approach to Diagnosis
Effective management of ALI often requires a multidisciplinary approach involving vascular surgeons, interventional radiologists, cardiologists, and critical care specialists. Early collaboration improves diagnostic accuracy and facilitates rapid therapeutic decisions.
Key Steps in the Diagnostic Workflow
- Immediate clinical assessment and limb examination.
- Bedside Doppler evaluation to confirm arterial flow compromise.
- Laboratory investigations to rule out underlying coagulopathies or systemic causes.
- CTA, MRA, or DSA for precise localization of arterial obstruction.
- Risk stratification using clinical scoring and imaging results.
Prompt diagnosis is critical; guidelines recommend revascularization within 6 hours of symptom onset to maximize limb salvage.
Conclusion
Acute Limb Ischemia is a medical emergency requiring rapid recognition, accurate diagnosis, and immediate intervention. A combination of thorough clinical evaluation, laboratory investigations, and imaging studies enables early detection and guides effective treatment. Healthcare providers must maintain a high index of suspicion, especially in patients with cardiovascular risk factors or sudden onset limb pain.