Introduction
Tympanoplasty is a specialized ear surgery performed to repair a perforated eardrum (tympanic membrane) or address issues in the middle ear bones. When left untreated, eardrum perforations can lead to hearing loss, frequent infections, and chronic ear discharge. Tympanoplasty helps restore hearing, prevents recurrent infections, and improves overall ear health.
What Is Tympanoplasty?
Tympanoplasty is a surgical procedure designed to reconstruct a damaged eardrum or middle ear ossicles. It is commonly recommended for
- Chronic ear infections
- Trauma-related eardrum perforations
- Hearing loss due to middle ear damage
- Recurrent ear discharge
- Cholesteatoma (abnormal skin growth behind the eardrum)
Doctors classify tympanoplasty into different types based on the extent of repair required. Understanding these types helps patients make informed decisions about the treatment recommended by their ENT specialist.
Types of Tympanoplasty
Tympanoplasty is categorized according to the level of damage and the surgical approach used. The most commonly used classification system is Wullstein’s classification, which includes five types.
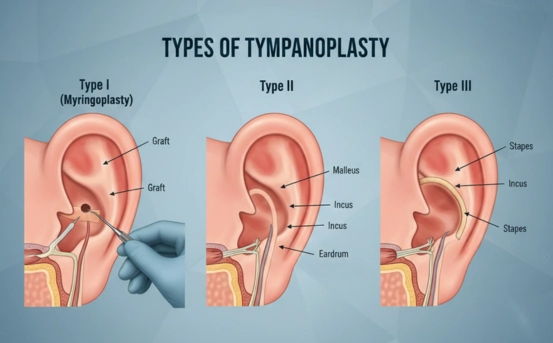
- Type I Tympanoplasty (Myringoplasty) :- Repair of the eardrum only, without involving the middle ear bones.
Type I tympanoplasty is performed when the ossicles (tiny hearing bones) are intact and functioning normally. The surgeon places a graft usually fascia, cartilage, or perichondrium under the perforated eardrum to close the hole.
This helps restore hearing and prevents infections caused by repeated exposure of the middle ear.
Ideal for
- Small to medium perforations
- Chronic perforations after infections
- Traumatic eardrum injury
- Patients with intact middle ear structures
Benefits
- Quick recovery
- High success rate
- Minimal surgical intervention
- Type II Tympanoplasty :- Repair of the eardrum along with partial reconstruction of the malleus (first middle ear bone).
In cases where the malleus is partially damaged or eroded due to chronic infections, Type II tympanoplasty is recommended. The surgeon reconstructs the malleus and attaches the graft securely to improve sound conduction.
Ideal for
- Partial ossicular chain damage
- Patients with limited malleus erosion
Benefits
- Restores sound transmission
- Prevents further middle ear complications
- Type III Tympanoplasty :- Reconstruction when the malleus and incus (two middle ear bones) are damaged or absent.
In this type, the surgeon connects the eardrum graft directly to the head of the stapes (third middle ear bone). This helps bypass the damaged ossicles and maintain adequate hearing function.
Ideal for
- Severe ossicular damage
- Chronic middle ear disease
- Patients who have undergone previous ear surgeries
Benefits:
- Effective for advanced middle ear damage
- Helps maintain functional hearing
- Type IV Tympanoplasty :- Protecting the round window of the inner ear and preserving residual hearing.
Type IV tympanoplasty is performed when only the stapes footplate remains intact. The surgeon reconstructs the ear structure in a way that shields the round window and improves hearing by preventing sound energy loss.
Ideal for
- Extensive middle ear erosion
- Patients with cholesteatoma
- Advanced chronic otitis media
Benefits:
- Prevents inner ear damage
- Allows better sound transmission even with severe ossicular loss
- Type V Tympanoplasty :- Specialized reconstruction for cases needing stapes mobilization or fenestration.
This procedure is rarely performed today due to advancements in modern surgical techniques but may be used in specific cases where the stapes footplate is fixed. Surgeons create alternate pathways for sound transmission to improve hearing.
Ideal for
- Severe otosclerosis
- Cases where traditional tympanoplasty techniques fail
Benefits
- Helps restore hearing when stapes mobility is compromised
How Surgeons Choose the Right Type of Tympanoplasty
ENT surgeons consider several factors before deciding on the appropriate tympanoplasty type
- Size and location of the eardrum perforation
- Condition of the middle ear ossicles
- Presence of chronic infection or cholesteatoma
- Patient’s hearing level and medical history
- Previous ear surgeries
A detailed ear examination, audiometry test, CT scan (if needed), and endoscopic evaluation help determine the most suitable technique.
Recovery After Tympanoplasty
Recovery varies depending on the type and complexity of surgery. Typical healing includes
- Mild pain for a few days
- Ear packing removal after 1–2 weeks
- Avoiding water entry into the ear
- No nose blowing or heavy lifting for a few weeks
- Gradual improvement in hearing over 6–8 weeks
Most patients return to normal activities within a week, but complete healing may take several months.
Conclusion
Tympanoplasty is an effective procedure to repair eardrum perforations, improve hearing, and prevent recurrent infections. With multiple types ranging from simple eardrum repair to advanced ossicular reconstruction the surgery is tailored to match the patient’s specific ear condition.
Consulting an experienced ENT specialist ensures accurate diagnosis and the most suitable type of tympanoplasty for long-term ear health.