Introduction
Congenital anomalies of the uterus are developmental abnormalities that occur during fetal life when the female reproductive system does not form normally. These anomalies may remain unnoticed for years and are often discovered incidentally during evaluation for menstrual irregularities, infertility, recurrent pregnancy loss, or obstetric complications. Accurate diagnosis plays a crucial role in identifying the condition early, guiding treatment decisions, and improving reproductive outcomes.
Diagnosing a congenital uterine anomaly requires a careful combination of clinical evaluation, imaging techniques, and sometimes invasive procedures. Because symptoms can vary widely or be entirely absent, a systematic and thorough diagnostic approach is essential to ensure correct identification and appropriate management.
Diagnosis of Congenital Anomaly Uterus
- Clinical Evaluation and Medical History :- The diagnostic process usually begins with a detailed medical history and physical examination. Many individuals with uterine anomalies present with complaints such as irregular menstrual cycles, painful menstruation, difficulty conceiving, or repeated miscarriages. In adolescents, the condition may be suspected when menstruation does not begin at the expected age or is associated with severe pain. A gynecologist carefully evaluates menstrual patterns, reproductive history, pregnancy outcomes, and any prior gynecological procedures. A family history of reproductive anomalies or kidney abnormalities may also raise suspicion, as these conditions can be associated with uterine developmental disorders. While physical examination alone cannot confirm a uterine anomaly, it helps identify associated findings and determine the need for further investigation.
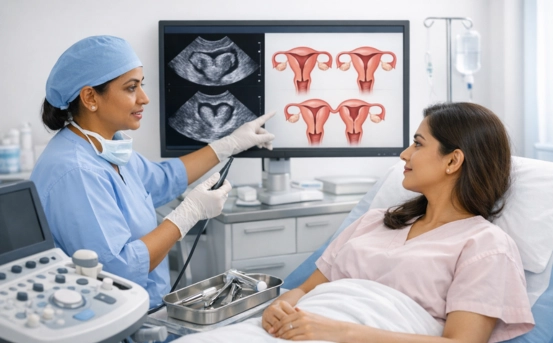
- Pelvic Ultrasound :- Pelvic ultrasound is usually the first imaging modality used in the diagnostic evaluation. It is widely available, non-invasive, and cost-effective. Transabdominal or transvaginal ultrasound allows visualization of the uterus, cervix, and ovaries, helping to identify abnormal uterine shape or size. Although standard ultrasound provides valuable initial information, its accuracy depends on operator expertise and patient factors. In some cases, ultrasound findings may be inconclusive, particularly when evaluating subtle structural abnormalities. However, it remains an essential screening tool and often guides the need for advanced imaging studies.
- Three-Dimensional Ultrasound :- Three-dimensional (3D) ultrasound has significantly improved the diagnosis of congenital uterine anomalies. Unlike traditional ultrasound, it provides a detailed view of the uterine cavity and outer uterine contour simultaneously. This allows clinicians to assess the internal structure with greater accuracy. 3D ultrasound is especially helpful in evaluating reproductive issues such as infertility or recurrent pregnancy loss. It is non-invasive, quick to perform, and highly reliable when conducted by trained professionals. Due to its diagnostic precision, 3D ultrasound has become one of the preferred methods for evaluating suspected uterine anomalies.
- Magnetic Resonance Imaging (MRI) :- Magnetic Resonance Imaging (MRI) is considered one of the most accurate diagnostic tools for congenital uterine anomalies. It offers excellent soft-tissue contrast and detailed images of the uterus, cervix, vagina, and surrounding structures without exposure to radiation. MRI is particularly useful when ultrasound findings are unclear or when associated abnormalities of the urinary tract are suspected. It provides comprehensive anatomical information, allowing precise assessment of uterine structure and orientation. Because of its high diagnostic accuracy, MRI is often used for confirmation and pre-treatment planning.
- Hysterosalpingography (HSG) :- Hysterosalpingography (HSG) is a specialized X-ray procedure commonly used during infertility evaluations. It involves injecting a contrast dye into the uterine cavity and fallopian tubes to assess their shape and patency. HSG can reveal abnormalities in the uterine cavity and identify structural irregularities. However, it only outlines the inner cavity and does not provide information about the outer uterine contour. As a result, HSG is often combined with other imaging methods to obtain a complete diagnostic picture.
- Hysteroscopy :- Hysteroscopy is a minimally invasive procedure that allows direct visualization of the uterine cavity using a thin, lighted instrument inserted through the cervix. It provides real-time images and enables precise evaluation of the internal uterine structure. This procedure is particularly valuable when imaging studies suggest an abnormal cavity or when patients experience unexplained infertility or recurrent pregnancy loss. In addition to diagnostic benefits, hysteroscopy allows for corrective procedures to be performed simultaneously if needed. However, it only evaluates the inside of the uterus and is often combined with laparoscopy for comprehensive assessment.
- Laparoscopy :- Laparoscopy is a minimally invasive surgical procedure used to visualize the external surface of the uterus and surrounding pelvic organs. It involves small incisions through which a camera is inserted into the abdominal cavity. This technique is often employed when non-invasive imaging results are inconclusive or when surgical correction is being considered. Laparoscopy allows accurate evaluation of the uterine shape, size, and orientation while also identifying any associated pelvic conditions. When combined with hysteroscopy, it offers a complete assessment of both internal and external uterine anatomy.
Evaluation of Associated Conditions
Congenital uterine anomalies may be associated with abnormalities in other organ systems, particularly the urinary tract. Therefore, renal imaging studies such as ultrasound or MRI may be recommended as part of the diagnostic workup.
Hormonal evaluations and genetic testing are not routinely required but may be considered in complex cases or when other developmental anomalies are suspected. A multidisciplinary approach involving gynecologists, radiologists, and reproductive specialists ensures comprehensive evaluation and accurate diagnosis.
Importance of Accurate Diagnosis
Accurate diagnosis of congenital uterine anomalies is critical for effective management. Misdiagnosis or delayed identification can lead to unnecessary treatments, persistent symptoms, or poor reproductive outcomes. Early detection allows healthcare providers to tailor treatment plans, counsel patients regarding fertility and pregnancy risks, and improve long-term reproductive health.
A precise diagnosis also helps differentiate congenital anomalies from acquired uterine conditions such as fibroids or adhesions, ensuring appropriate care.
Conclusion
The diagnosis of congenital anomalies of the uterus requires a systematic and thorough approach that combines clinical evaluation with advanced imaging and minimally invasive procedures. From pelvic ultrasound and MRI to hysteroscopy and laparoscopy, each diagnostic method plays a vital role in identifying structural abnormalities and guiding treatment decisions.
Because symptoms may be subtle or absent, a high index of suspicion is essential, particularly in individuals with infertility, menstrual irregularities, or recurrent pregnancy loss. With advancements in imaging technology and minimally invasive diagnostics, accurate identification has become more achievable than ever. Early and precise diagnosis not only improves reproductive outcomes but also enhances overall gynecological health and quality of life.