Introduction
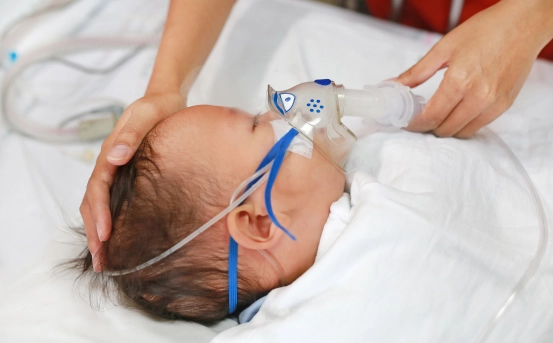
The Neonatal Intensive Care Unit (NICU) is a specialized unit designed to provide advanced medical care to critically ill or premature newborns. While most babies are born healthy and thrive without medical intervention, certain conditions and complications can necessitate NICU admission. Understanding the causes of advanced NICU care can help parents, caregivers, and healthcare providers prepare, prevent, and manage these situations more effectively.
Causes of Advanced NICU
- Premature Birth :- One of the most common reasons a newborn may require NICU care is premature birth, defined as delivery before 37 weeks of gestation. Premature babies often have underdeveloped organs, particularly the lungs, brain, and digestive system. This underdevelopment can lead to respiratory distress, difficulty maintaining body temperature, feeding issues, and increased susceptibility to infections. Several factors can contribute to premature birth, including maternal health conditions like hypertension, diabetes, or infections. Multiple pregnancies (twins, triplets, etc.) and complications like preterm labor or placental problems also increase the likelihood of early delivery. Babies born prematurely often require specialized monitoring, breathing support, and nutritional assistance in the NICU to ensure proper growth and development.
- Respiratory Distress Syndrome (RDS) :- Respiratory Distress Syndrome is a significant cause of advanced NICU admission, particularly in preterm infants. RDS occurs due to insufficient production of surfactant, a substance that helps the lungs stay inflated and facilitates normal breathing. Without adequate surfactant, the lungs collapse, making it extremely difficult for the newborn to breathe independently. Babies with RDS may present with rapid breathing, grunting sounds, flaring nostrils, and cyanosis (bluish skin due to lack of oxygen). Treatment often requires respiratory support, such as mechanical ventilation or Continuous Positive Airway Pressure (CPAP), as well as administration of surfactant therapy. Advanced NICU facilities are equipped to manage these critical respiratory challenges.
- Infections and Sepsis :- Newborns, especially those with low birth weight or premature birth, have underdeveloped immune systems, making them highly vulnerable to infections. Neonatal infections, including bacterial, viral, or fungal infections, can quickly become severe and lead to sepsis, a life-threatening condition where the body’s response to infection causes organ damage. Common sources of infection include maternal infections during pregnancy, complications during labor, or exposure to pathogens after birth. Signs of neonatal infection include fever, lethargy, poor feeding, respiratory distress, and abnormal heart rates. Advanced NICU care provides immediate antibiotic therapy, monitoring of vital signs, and supportive care to prevent further complications.
- Birth Asphyxia :- Birth asphyxia occurs when a newborn experiences a lack of oxygen before, during, or immediately after birth. Oxygen deprivation can result from complications such as umbilical cord problems, placental insufficiency, prolonged labor, or maternal health issues. The consequences of birth asphyxia can be severe, affecting the brain, heart, kidneys, and other vital organs. Infants may require NICU admission for oxygen therapy, mechanical ventilation, and close monitoring of neurological function. In some cases, therapeutic hypothermia (controlled cooling of the body) is used to reduce the risk of long-term brain injury.
- Low Birth Weight :- Low birth weight, defined as weighing less than 2,500 grams at birth, is a critical factor leading to advanced NICU admission. Low birth weight can result from premature birth, intrauterine growth restriction (IUGR), or maternal health conditions like malnutrition, high blood pressure, or infections during pregnancy. Infants with low birth weight are more prone to hypothermia, hypoglycemia (low blood sugar), infections, and breathing difficulties. NICU support includes maintaining optimal body temperature, nutritional support via intravenous fluids or feeding tubes, and close monitoring to prevent complications.
- Congenital Disorders and Birth Defects :- Some newborns are born with congenital disorders or birth defects that require immediate attention in an advanced NICU. These can range from heart defects and cleft palate to gastrointestinal malformations and metabolic disorders. Early detection through prenatal screenings or immediate postnatal diagnosis allows for timely intervention. Depending on the condition, NICU care may involve surgical interventions, medications, and close monitoring of vital functions. Advanced NICUs are equipped with the specialized technology and trained personnel to manage these complex cases.
- Maternal Health Complications :- The health of the mother plays a significant role in determining whether a newborn may need NICU care. Conditions such as gestational diabetes, preeclampsia, infections, and thyroid disorders can impact fetal development and increase the risk of complications at birth. Maternal lifestyle factors such as smoking, alcohol consumption, and drug use during pregnancy also contribute to neonatal complications. Advanced NICU care ensures that infants born to high-risk mothers receive immediate and comprehensive care to stabilize their condition and support growth and development.
- Neonatal Hypoglycemia :- Hypoglycemia, or low blood sugar, is another common reason for NICU admission. Newborns, particularly those with low birth weight, premature birth, or maternal diabetes, may experience difficulty regulating blood sugar levels. Symptoms include jitteriness, lethargy, poor feeding, and seizures. NICU interventions involve frequent monitoring of blood glucose, intravenous glucose administration, and supportive care to prevent long-term neurological complications.
- Advanced NICU Technologies and Support :- Modern NICUs are equipped with cutting-edge technology to manage these conditions effectively. Ventilators, incubators, infusion pumps, advanced monitoring systems, and specialized feeding equipment ensure that critically ill newborns receive optimal care. Additionally, NICU teams include neonatologists, nurses, respiratory therapists, and nutritionists working together to provide comprehensive support for both the baby and the family.
Conclusion
Advanced NICU admissions are often the result of a combination of factors including premature birth, respiratory distress, infections, birth asphyxia, low birth weight, congenital disorders, and maternal health complications. Awareness of these causes is crucial for expecting parents, caregivers, and healthcare professionals to minimize risks and ensure timely interventions.
While the need for NICU care can be stressful for families, modern advancements in neonatal medicine significantly improve survival rates and long-term outcomes for critically ill newborns. Proactive prenatal care, timely medical intervention, and a supportive NICU environment play essential roles in safeguarding the health of these vulnerable infants.