Introduction
Epidural hematoma is a serious medical condition that occurs when blood accumulates between the skull and the outer layer of the brain’s protective covering, known as the dura mater. Prompt diagnosis and treatment are critical because this condition can rapidly become life-threatening. Surgery is often required to remove the accumulated blood and relieve pressure on the brain. Understanding the causes of epidural hematoma surgery is essential for prevention, early detection, and timely medical intervention.
What is Epidural Hematoma Surgery?
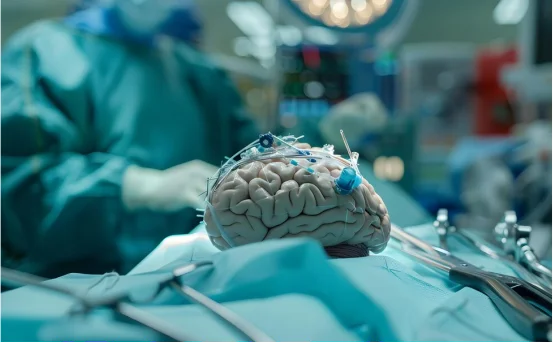
Epidural hematoma surgery, often referred to as a craniotomy for hematoma evacuation, involves the surgical removal of blood that has pooled in the epidural space. The procedure helps reduce pressure on the brain, preventing permanent damage and potentially saving a patient’s life. The surgery typically involves creating a small opening in the skull to access and remove the hematoma. Early intervention significantly improves the chances of recovery.
Common Causes of Epidural Hematoma Surgery
Several factors can lead to the development of an epidural hematoma that necessitates surgical intervention. Understanding these causes can help in reducing risk and promoting timely treatment.
- Head Trauma from Accidents :- One of the most common causes of epidural hematomas is head trauma resulting from accidents, such as road traffic collisions, falls, or sports injuries. A strong impact can rupture the blood vessels between the skull and dura mater, causing blood to accumulate rapidly. In many cases, immediate surgery is required to prevent brain compression and life-threatening complications.
- Skull Fractures :- Skull fractures, especially in the temporal or parietal regions, are strongly associated with epidural hematomas. When the bone breaks, it can tear the middle meningeal artery, leading to rapid blood accumulation. Surgical intervention is usually urgent, as untreated hematomas can lead to severe neurological damage or even death.
- Post-Surgical Complications :- Although rare, some patients may develop an epidural hematoma following neurosurgery or other cranial procedures. Postoperative bleeding can increase intracranial pressure, necessitating a secondary surgery to evacuate the hematoma and stabilize the patient. Continuous monitoring and imaging are crucial in these cases.
- Blood Clotting Disorders :- Patients with clotting disorders, such as hemophilia or those on long-term anticoagulant therapy, are at higher risk for spontaneous or trauma-induced epidural hematomas. Even minor head injuries can lead to excessive bleeding, requiring surgical intervention to prevent brain injury.
- Violent Impacts or Assaults :- Physical assaults or violent impacts to the head can also cause epidural hematomas. Blunt force trauma can rupture arteries or veins near the skull, leading to the accumulation of blood. Rapid surgical treatment is often necessary to alleviate pressure on the brain.
Symptoms Indicating the Need for Surgery
Recognizing the symptoms of an epidural hematoma is vital for early intervention. Patients often exhibit a “lucid interval,” where they regain consciousness briefly after injury but deteriorate quickly afterward. Common symptoms include:
- Severe headache and nausea
- Vomiting and dizziness
- Confusion or drowsiness
- Weakness or numbness on one side of the body
- Seizures or loss of consciousness
If these symptoms appear after a head injury, urgent medical attention is required. Delaying surgery can significantly increase the risk of permanent brain damage or death.
Diagnosis and Medical Evaluation
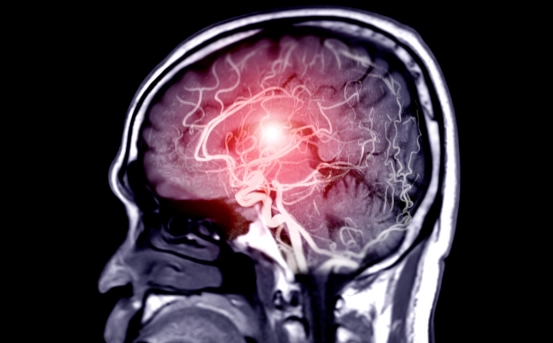
Diagnosis of epidural hematoma typically involves imaging studies such as a CT scan or MRI. These imaging techniques allow doctors to pinpoint the location and size of the hematoma. Once diagnosed, a neurosurgeon evaluates the patient to determine the need for surgical intervention. The decision is often based on the size of the hematoma, the patient’s neurological status, and the rate at which the blood is accumulating.
Prevention and Awareness
While not all cases of epidural hematomas are preventable, certain measures can reduce the risk:
- Wearing protective gear during sports or high-risk activities
- Using seat belts and child safety seats in vehicles
- Avoiding falls by ensuring home safety, especially for the elderly
- Monitoring patients on anticoagulants closely for signs of head injury
Awareness of symptoms and prompt medical attention are key to improving outcomes.
Conclusion
Epidural hematoma is a life-threatening condition that requires immediate attention, and surgery is often the most effective treatment to prevent serious brain injury. The causes range from traumatic accidents and skull fractures to clotting disorders and postoperative complications. By understanding these causes, recognizing early symptoms, and seeking timely medical care, patients can significantly improve their recovery outcomes.