Introduction
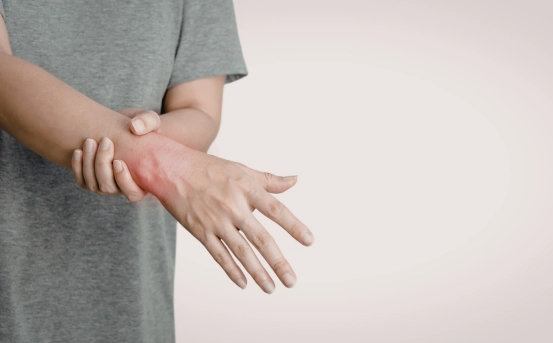
Raynaud’s disease, also called Raynaud’s phenomenon, is a condition in which blood flow to certain parts of the body usually fingers and toes is restricted in response to cold temperatures or emotional stress. This restricted blood flow causes the affected areas to turn white, blue, or red, often accompanied by pain, numbness, or tingling. Understanding the causes of Raynauds disease helps patients and caregivers identify triggers, manage symptoms effectively, and seek timely medical care when necessary. The condition is generally categorized into primary Raynaud’s (occurring on its own) and secondary Raynaud’s (caused by another underlying condition).
Causes of Raynauds Disease
Primary Raynaud’s, also called idiopathic Raynaud’s, occurs without any identifiable underlying medical condition. The exact cause is not fully understood, but several factors are thought to contribute:
- Overactive Blood Vessel Response: In primary Raynaud’s, the small arteries in the fingers and toes overreact to cold or stress by narrowing excessively, reducing blood flow temporarily.
- Nerve Sensitivity: The nerves that regulate blood vessel constriction may be overly sensitive, triggering spasms that cause color changes and discomfort.
- Genetic Predisposition: A family history of Raynaud’s may increase the likelihood of developing the condition, suggesting a hereditary component.
- Environmental Factors: Cold weather or exposure to sudden temperature changes is a common trigger. Emotional stress can also induce episodes.
Primary Raynaud’s is usually mild and does not lead to serious complications. Symptoms are often manageable with lifestyle modifications and protective measures.
Secondary Causes of Raynaud’s Disease
Secondary Raynaud’s, also called Raynaud’s phenomenon, occurs due to an underlying health condition or external factor. It tends to be more severe than primary Raynaud’s and can lead to complications such as ulcers or tissue damage. Common causes include:
- Connective Tissue Disorders: Conditions such as scleroderma, lupus, or rheumatoid arthritis can damage blood vessels, increasing susceptibility to Raynaud’s attacks.
- Blood Vessel Diseases: Diseases affecting the arteries, such as atherosclerosis or Buerger’s disease, can limit blood flow and trigger symptoms.
- Repetitive Trauma or Vibration: Jobs or activities that involve repetitive motion or the use of vibrating tools (like jackhammers or power tools) can damage blood vessels and cause secondary Raynaud’s.
- Medications: Certain medications that constrict blood vessels, including beta-blockers, migraine medications, and some chemotherapy drugs, can trigger Raynaud’s symptoms.
- Smoking: Nicotine causes blood vessel constriction and can worsen Raynaud’s attacks.
- Hormonal Factors: Hormonal changes, such as those during menopause or due to thyroid disorders, may influence blood vessel behavior.
- Occupational or Environmental Exposure: Frequent exposure to cold environments or chemicals that damage blood vessels, such as vinyl chloride, can lead to secondary Raynaud’s.
- Nerve Injuries: Trauma or nerve compression in the hands or feet can disrupt normal blood vessel control and trigger Raynaud’s episodes.
Other Risk Factors
Certain factors increase the likelihood of developing Raynaud’s disease:
- Age: Most commonly starts between 15 and 30 years.
- Gender: More common in women than men.
- Family History: A parent or sibling with Raynaud’s increases risk.
- Climate: Living in colder climates increases the frequency of attacks.
Conclusion
Raynaud’s disease occurs due to a combination of overactive blood vessel responses, nerve sensitivity, genetic predisposition, and environmental triggers in primary cases. Secondary Raynaud’s arises from underlying health conditions, trauma, medication use, or vascular damage. Identifying the cause is critical for managing the condition effectively. While primary Raynaud’s can often be controlled with lifestyle adjustments, secondary Raynaud’s requires addressing the underlying disease along with symptom management. Consulting an experienced physician or vascular specialist ensures accurate diagnosis, proper care, and prevention of serious complications such as ulcers or tissue damage. Although Raynaud’s surgery is not necessary for every patient diagnosed with Raynaud’s phenomenon, it becomes a vital option for those experiencing frequent or debilitating attacks, chronic pain, and complications that significantly affect daily life. The surgery provides hope for patients who have exhausted conservative treatments and continue to suffer from limited hand or foot function, recurrent injuries, or poor wound healing due to inadequate blood supply. In addition to improving blood flow, the procedure may also help patients regain dexterity, strength, and confidence in performing routine activities, which are often disrupted by recurrent Raynaud’s attacks.