Introduction
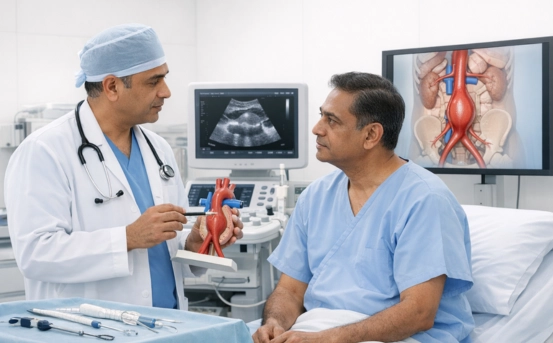
Abdominal Aortic Aneurysm (AAA) is a potentially life-threatening condition that occurs when the lower part of the aorta, the main blood vessel supplying blood to the body, becomes enlarged or weakened. Timely diagnosis is crucial because an untreated abdominal aortic aneurysm can rupture, leading to massive internal bleeding. Early detection not only saves lives but also allows doctors to recommend preventive treatment before complications arise. Here we explain the symptoms, risk factors, and the complete diagnostic process for abdominal aortic aneurysm using modern imaging technologies. This 900-word blog is designed to help patients, caregivers, and healthcare professionals understand how AAA is detected and why timely screening matters.
What Is an Abdominal Aortic Aneurysm?
An abdominal aortic aneurysm is a bulge that develops in the lower section of the aorta. Over time, the vessel wall weakens, causing it to enlarge. Small aneurysms may remain stable for years, but larger or fast-growing aneurysms increase the risk of rupture. Because AAA usually develops silently, diagnosis often happens during routine check-ups or imaging tests done for other medical reasons. This is why knowing the risk factors and getting screened at the right time is essential.
Common Symptoms of Abdominal Aortic Aneurysm
In most cases, abdominal aortic aneurysms have no symptoms. However, some people may experience
- A deep, persistent pain in the abdomen or lower back
- A pulsing sensation near the navel
- Sudden, severe pain indicating possible rupture
Once symptoms appear, urgent medical evaluation is necessary.
Who Should Get Screened for AAA?
Screening is the most effective way to diagnose abdominal aortic aneurysm early. Certain groups are at higher risk
- Men aged 65 to 75, especially those who have smoked
- People with a family history of abdominal aortic aneurysm
- Individuals with hypertension, high cholesterol, or cardiovascular disease
- Patients with atherosclerosis
- Smokers, current or past
Doctors usually recommend one-time screening for older men, while high-risk individuals may need repeat tests.
Diagnosis of Abdominal Aortic Aneurysms
Accurate diagnosis is essential for determining the size, shape, and severity of an abdominal aortic aneurysm. Several advanced imaging tests are used to detect AAA early. Here are the most commonly used diagnostic methods
- Abdominal Ultrasound (Primary Screening Test) :- An abdominal ultrasound is the most widely used and preferred test for the early detection of AAA. It is
- Non-invasive
- Painless
- Quick
- Highly accurate
- Affordable
During the scan, sound waves create a real-time image of the abdominal aorta. Ultrasound can identify the exact diameter of the aorta and help doctors decide whether monitoring or treatment is needed. It is typically the first-choice test for routine screening.
- CT Scan (Computed Tomography Scan) :- A CT scan provides detailed 3D images of the abdominal aorta and surrounding organs. Doctors recommend CT scans when
- An aneurysm is suspected to be large
- The ultrasound results are unclear
- Surgery or stent placement is being planned
A contrast dye is often used to highlight the blood vessels. CT scans are extremely accurate and help determine the exact shape and extent of the aneurysm.
- MRI Scan (Magnetic Resonance Imaging) :- MRI is another non-invasive test that gives clear and detailed images of the aorta without radiation exposure. MRI scans are helpful for
- Patients who cannot undergo CT scan due to contrast allergies
- Long-term monitoring of aneurysms
- Mapping the aorta for surgical planning
Although MRI takes longer, it offers excellent soft tissue imaging with high precision.
- Physical Examination :- While imaging tests are essential, a physical exam can sometimes help detect large aneurysms. During examination, the doctor may feel a pulsating mass in the abdomen. However, because many aneurysms are small or deep inside the body, imaging is necessary for a confirmed diagnosis.
- Blood Tests :- There is no specific blood test to detect AAA, but doctors may order
- Cholesterol tests
- Inflammatory markers
- Kidney function tests
- Glucose levels
These tests help evaluate overall health and determine a patient’s risk for complications and suitability for surgery.
How Doctors Evaluate an Abdominal Aortic Aneurysm
Once an aneurysm is detected, doctors assess several important factors
Aneurysm Size
- Small (<4 cm): Usually monitored every 6–12 months
- Medium (4–5.4 cm): More frequent monitoring
- Large (≥5.5 cm): Surgery often recommended
Growth Rate :- An aneurysm growing more than 0.5 cm in six months indicates higher rupture risk.
Shape and Location :- Fusiform aneurysms (uniform bulge) are more common, while saccular aneurysms (localized bulge) may have higher rupture risk.
Risks of an Undiagnosed Abdominal Aortic Aneurysm
Ignoring or missing the diagnosis of AAA can lead to dangerous outcomes, such as
- Aortic rupture, causing internal bleeding
- Blood clots that can block arteries
- Organ damage
- Life-threatening shock
Early diagnosis significantly reduces these risks, allowing timely intervention through monitoring or surgery.
Why Early Diagnosis Matters
Early detection of abdominal aortic aneurysm allows doctors to
- Track aneurysm growth with periodic imaging
- Recommend lifestyle changes to reduce risk
- Plan minimally invasive surgery, such as EVAR (Endovascular Aneurysm Repair), if needed
- Prevent rupture and save lives
AAA remains silent until advanced stages, making routine screening essential for high-risk individuals.
Conclusion
The diagnosis of an abdominal aortic aneurysm relies on advanced imaging techniques such as ultrasound, CT scan, and MRI. Early detection dramatically improves outcomes, helping patients avoid life-threatening complications. If you fall into a high-risk category or experience symptoms like persistent abdominal or back pain, speak to your doctor about getting screened. Prompt diagnosis is the most powerful tool in preventing rupture and ensuring long-term health.