Introduction
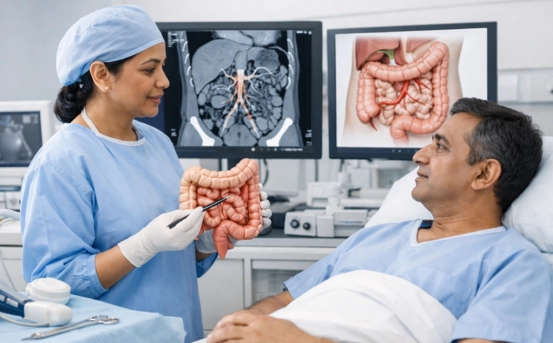
Mesenteric ischemia is a serious and potentially life-threatening condition caused by reduced blood flow to the small intestine. Timely diagnosis is crucial to prevent irreversible intestinal damage, sepsis, and even death. Here will provides an in-depth look at the diagnosis of mesenteric ischemia, including its types, symptoms, risk factors, and the key investigative tools used by healthcare professionals.
Understanding Mesenteric Ischemia
Mesenteric ischemia occurs when blood flow to the intestines is compromised. There are two main types
- Acute Mesenteric Ischemia (AMI): A sudden reduction in blood supply, often caused by embolism, thrombosis, or low blood pressure. AMI requires urgent intervention.
- Chronic Mesenteric Ischemia (CMI): Gradual narrowing of the mesenteric arteries, usually due to atherosclerosis. Symptoms develop slowly and often include postprandial abdominal pain and unintentional weight loss.
Early recognition is essential because delays in diagnosis can lead to intestinal necrosis, multi-organ failure, and high mortality rates.
Risk Factors for Mesenteric Ischemia
Understanding risk factors can help healthcare providers identify patients at higher risk
- Atrial fibrillation, myocardial infarction, or atherosclerosis
- Hypercoagulable states
- Recent major surgery or trauma
- Low blood pressure or shock
- Advanced age
- Smoking and high cholesterol
Common Symptoms Suggesting Mesenteric Ischemia
The symptoms vary between acute and chronic forms
- Acute Mesenteric Ischemia
- Severe abdominal pain, often out of proportion to physical examination findings
- Nausea and vomiting
- Diarrhea or bloody stools
- Rapid heart rate and low blood pressure
- Chronic Mesenteric Ischemia
- Abdominal pain after meals (intestinal angina)
- Fear of eating due to pain
- Unintended weight loss
- Bloating and diarrhea
Diagnosis of Mesenteric Ischemia
Diagnosing mesenteric ischemia is challenging because symptoms are often nonspecific. Physicians rely on a combination of clinical evaluation, laboratory tests, and advanced imaging techniques.
- Clinical Evaluation :- A detailed patient history and physical examination are the first steps. Key indicators include
- Sudden, severe abdominal pain in AMI
- History of cardiovascular disease or atrial fibrillation
- Signs of peritonitis in advanced cases
Early suspicion is critical, as mesenteric ischemia can progress rapidly.
- Laboratory Tests :- While no blood test can definitively diagnose mesenteric ischemia, certain markers can raise suspicion
- Complete Blood Count (CBC): May show elevated white blood cells indicating inflammation.
- Serum Lactate: Elevated levels suggest tissue hypoxia and ischemia.
- D-dimer Test: Can support the diagnosis of thrombotic or embolic events.
- Arterial Blood Gas (ABG): Metabolic acidosis may indicate severe ischemia.
- Imaging Studies :- Imaging plays a central role in confirming mesenteric ischemia and guiding treatment.
- Computed Tomography Angiography (CTA) :- CTA is the preferred imaging modality for acute mesenteric ischemia. It provides detailed visualization of the mesenteric arteries and can identify blockages, arterial narrowing, and intestinal wall changes. CTA also helps detect complications like bowel necrosis or perforation.
- Magnetic Resonance Angiography (MRA) :- MRA is useful for patients with contraindications to iodinated contrast. It helps in assessing chronic mesenteric ischemia and vessel patency.
- Duplex Ultrasonography :- This non-invasive test evaluates blood flow in the mesenteric arteries. It is particularly useful for screening and follow-up in chronic cases.
- Conventional Angiography :- Although more invasive, catheter-based angiography can be both diagnostic and therapeutic. It allows for interventions like thrombolysis or stenting in selected patients.
- Endoscopic Evaluation :- In some cases, endoscopy may be used to assess bowel viability or rule out other causes of abdominal pain. Findings like mucosal edema, ulceration, or gangrene can suggest ischemia.
- Exploratory Laparoscopy or Surgery :- When imaging is inconclusive and symptoms persist, exploratory laparoscopy or laparotomy may be necessary to directly visualize the intestines. This approach is particularly critical in suspected acute mesenteric ischemia with signs of peritonitis.
Challenges in Diagnosing Mesenteric Ischemia
- Nonspecific symptoms: Early-stage ischemia may mimic other gastrointestinal disorders.
- Rapid progression: Acute cases can deteriorate quickly, leaving little time for extensive testing.
- Comorbidities: Conditions like diabetes or chronic heart disease can mask symptoms.
Early recognition and a high index of suspicion are essential to improve patient outcomes.
Conclusion
Mesenteric ischemia is a life-threatening condition requiring prompt diagnosis. A combination of clinical evaluation, laboratory markers, and advanced imaging ensures accurate detection and timely intervention. For patients with cardiovascular risk factors or sudden unexplained abdominal pain, early consultation with a specialist can save lives.
Healthcare providers should maintain a high index of suspicion for mesenteric ischemia, especially in acute presentations, as early diagnosis significantly reduces the risk of complications. Advanced diagnostic tools like CTA, MRA, and angiography play a pivotal role in confirming the diagnosis and guiding treatment strategies.