Introduction
Tympanoplasty is a specialized surgical procedure performed to repair a perforated eardrum (tympanic membrane) or reconstruct middle ear structures to restore hearing. While the surgery itself is highly effective, its success largely depends on a thorough and accurate pre-surgical diagnosis. Understanding how doctors determine the need for the diagnosis of tympanoplasty can help patients feel more confident and prepared as they begin their treatment journey.
Understanding When Tympanoplasty Is Needed
An eardrum perforation can occur due to chronic ear infections, trauma, sudden pressure changes, or previous surgeries. While many perforations heal naturally, persistent or large holes in the eardrum may require tympanoplasty. Diagnosing the need for surgery typically begins when a patient presents with symptoms such as
- Hearing loss
- Recurrent ear infections
- Ear discharge (otorrhea)
- Pain or discomfort
- Difficulty hearing in noisy environments
- A feeling of fullness or pressure in the ear
These symptoms alert ENT specialists (otolaryngologists) to perform further evaluation.
Diagnosis of Tympanoplasty
- Medical History Review :- A detailed medical history is the first step. The ENT specialist discusses
- Duration and severity of symptoms
- Past ear infections or chronic otitis media
- Previous ear surgeries
- Trauma to the ear
- Exposure to loud noise
- History of allergies or sinus issues
- Any prior treatments or medications used
This information helps doctors understand underlying causes and assess whether a perforation is long-standing or recent.
- Physical Examination :- A comprehensive ear examination provides the clearest initial insight into the condition of the eardrum.
- Otoscopy :- Using a handheld otoscope, the doctor examines the ear canal and tympanic membrane. They look for
- Size, location, and shape of the perforation
- Signs of infection or inflammation
- Scarring or thickening (tympanosclerosis)
- Fluid buildup behind the eardrum
A clear view of the perforation helps determine whether simple treatment or surgical repair is appropriate.
- Pneumatic Otoscopy :- This tool allows the doctor to see how well the eardrum moves when air pressure changes. Limited mobility often indicates fluid, infection, or other complications.
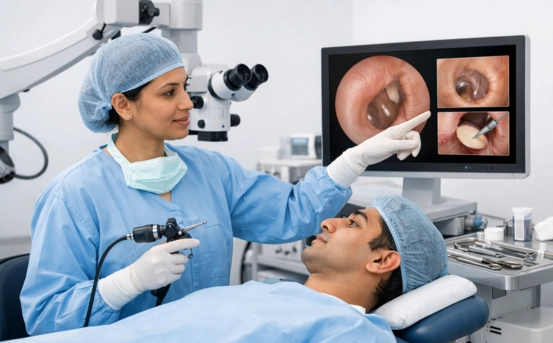
- Microscopic Ear Examination :- For more precision, many ENT specialists use an operating microscope. This allows high-magnification evaluation of
- Very small perforations
- Middle ear structures
- Presence of cholesteatoma (abnormal skin growth)
- Condition of the ossicles (ear bones)
This step is crucial, as cholesteatoma or ossicle damage may require additional procedures alongside tympanoplasty.
- Hearing Tests (Audiometry) :- Audiological evaluation is one of the most important diagnostic components. It determines how much hearing has been affected and helps the surgeon plan the procedure.
- Pure-Tone Audiometry :- This test measures the patient’s hearing thresholds at different sound frequencies. It shows whether the hearing loss is conductive (related to eardrum or middle ear issues), sensorineural (inner ear damage), or mixed.
- Speech Audiometry :- Assesses the patient’s ability to recognize and understand speech at various volumes.
- Tympanometry :- This measures how the eardrum responds to air pressure changes. A flat or abnormal tympanogram may indicate eardrum perforation or middle ear dysfunction. These tests provide baseline hearing levels and help the surgeon predict the hearing improvement possible after tympanoplasty.
- Imaging Tests (If Required) :- Imaging is not needed in every tympanoplasty case, but may be recommended when complications or unclear findings are present.
CT (Computed Tomography) Scan :- A CT scan of the temporal bone helps identify:
- Middle ear fluid
- Ossicular chain damage
- Mastoid infections
- Presence of cholesteatoma
- Anatomical variations that may affect surgery
CT imaging ensures the surgeon has a complete map of the patient’s ear anatomy before proceeding.
- Evaluation of Infection Status :- Active infection must be controlled before tympanoplasty. The ENT specialist checks for
- Persistent discharge
- Bacterial or fungal growth
- Swelling or redness
If an active infection is detected, antibiotic or antifungal treatment is given first. Surgery is typically scheduled once the ear remains dry for several weeks.
- Eustachian Tube Function Assessment :- Proper Eustachian tube function is essential for ear pressure regulation. Dysfunction can compromise tympanoplasty outcomes. Doctors evaluate
- Patient’s ability to equalize pressure
- History of sinus or nasal issues
- Allergies
- Any signs of blockage or inflammation
Sometimes, additional treatments are recommended before surgery to improve Eustachian tube function.
- Pre Surgical Counseling and Planning :- Once the diagnosis is complete, the ENT specialist discusses
- Type of tympanoplasty required (type I, II, or III)
- Expected hearing improvement
- Risks and benefits
- Recovery timeline
This helps the patient make an informed decision and prepare for surgery confidently.
Conclusion
Diagnosis of tympanoplasty is a detailed and multi-step process involving medical history analysis, physical examination, advanced hearing tests, microscopic evaluation, and sometimes imaging. Accurate diagnosis ensures that the underlying problem is clearly understood and that tympanoplasty offers the best chance of restoring hearing, preventing infections, and improving ear health.