Introduction
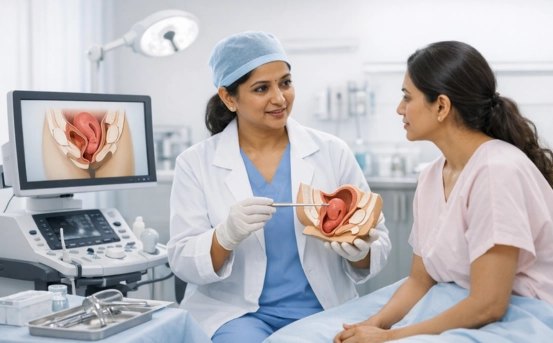
Vaginal descent, also commonly referred to as pelvic organ prolapse, is a condition where the pelvic organs, such as the bladder, uterus, or rectum, descend into or outside the vaginal canal due to weakened pelvic floor muscles. This condition can affect women of all ages but is most prevalent in postmenopausal women and those who have undergone childbirth. Early diagnosis is crucial to manage symptoms effectively, prevent complications, and improve the quality of life. We will discuss the methods used for the diagnosis of vaginal descent, signs to watch for, and the importance of timely medical consultation.
Understanding Vaginal Descent
Vaginal descent occurs when the muscles, ligaments, and connective tissues supporting the pelvic organs weaken, causing one or more organs to drop from their normal positions. Depending on the organ affected, vaginal descent may be classified as
- Cystocele: Descent of the bladder into the front wall of the vagina.
- Rectocele: Bulging of the rectum into the back wall of the vagina.
- Uterine prolapse: Descent of the uterus into the vaginal canal.
- Enterocele: Herniation of the small intestine into the upper vagina.
Common risk factors include vaginal childbirth, aging, menopause, obesity, chronic coughing, and heavy lifting. Women may experience symptoms such as a feeling of pressure in the pelvic area, urinary incontinence, bowel dysfunction, or even visible protrusion of tissue from the vagina.
Signs and Symptoms to Watch For
Early recognition of vaginal descent is critical for effective treatment. Symptoms may include
- A feeling of heaviness or pressure in the pelvic area.
- Difficulty in urination or frequent urinary tract infections.
- Constipation or difficulty with bowel movements.
- Pain or discomfort during sexual intercourse.
- Noticeable bulge or tissue protrusion from the vaginal opening.
Experiencing any of these symptoms warrants a consultation with a gynecologist or pelvic health specialist. Early evaluation can prevent progression and help select appropriate treatment options.
Clinical Examination
The diagnosis of vaginal descent begins with a detailed medical history and physical examination. A clinician will assess
- Medical and Obstetric History: Information about pregnancies, childbirth method, prior pelvic surgeries, and urinary or bowel issues.
- Symptom Evaluation: The severity and frequency of pelvic pressure, urinary incontinence, or bowel dysfunction.
- Pelvic Examination: A visual and manual examination of the vagina while the patient is in different positions, often during Valsalva maneuver (straining as if to defecate) to identify the extent of prolapse.
During the pelvic exam, the doctor will classify the prolapse using the Pelvic Organ Prolapse Quantification (POP-Q) system, which measures the descent of vaginal walls and organs in centimeters. This system helps standardize diagnosis and guides treatment planning.
Imaging and Advanced Diagnostic Techniques
While most cases of vaginal descent can be diagnosed clinically, imaging tests may be recommended in complex cases or when the extent of organ prolapse is uncertain. Common imaging techniques include
- Ultrasound: Transvaginal or transperineal ultrasound can assess the position of pelvic organs and detect abnormalities in the bladder, uterus, and rectum.
- Magnetic Resonance Imaging (MRI): MRI provides detailed images of the pelvic floor muscles, connective tissue, and organs. It is particularly helpful in complex prolapse cases or when surgical planning is required.
- Defecography: A specialized X-ray test to evaluate rectal prolapse and its impact on bowel function.
These advanced diagnostic tools complement the clinical exam, especially when symptoms are atypical or when previous treatments have failed.
Urodynamic Testing
Women with vaginal descent often experience urinary incontinence or other bladder dysfunctions. Urodynamic studies may be recommended to assess bladder function, urinary flow, and pressure. These tests help distinguish between prolapse-related urinary issues and other underlying bladder conditions, ensuring precise diagnosis and treatment.
Importance of Early Diagnosis
Early detection of vaginal descent offers several benefits
- Prevention of Progression: Timely diagnosis can prevent worsening prolapse and associated complications.
- Customized Treatment Planning: Physicians can recommend non-surgical options, such as pelvic floor exercises or pessary devices, or surgical interventions when necessary.
- Improved Quality of Life: Addressing prolapse symptoms early reduces discomfort, urinary or bowel issues, and enhances sexual health.
Ignoring the symptoms of vaginal descent can lead to severe prolapse, recurrent infections, and a significant decrease in overall well-being.
Treatment Planning Based on Diagnosis
Once vaginal descent is diagnosed, treatment is tailored to the severity of prolapse, symptoms, and patient’s preferences. Options include
- Conservative Management: Pelvic floor exercises (Kegels), lifestyle modifications, and vaginal pessaries.
- Medical Management: Hormonal therapies may be prescribed in postmenopausal women to strengthen vaginal tissues.
- Surgical Treatment: For severe prolapse, surgical correction such as vaginal or abdominal repair may be recommended.
Accurate diagnosis ensures the most effective treatment, whether conservative or surgical, and helps prevent recurrence.
When to Consult a Specialist
Women experiencing pelvic pressure, urinary or bowel difficulties, or noticeable vaginal bulges should seek gynecological evaluation promptly. Regular gynecologic check-ups, especially after childbirth or during menopause, can aid in early detection and better management of vaginal descent.
Conclusion
The diagnosis of vaginal descent is a crucial step in maintaining women’s pelvic health. Through a combination of clinical evaluation, imaging studies, and specialized tests, healthcare providers can accurately assess the extent of prolapse and recommend effective treatment options. Early detection not only alleviates symptoms but also enhances quality of life, reduces complications, and empowers women to take control of their pelvic health.Identify critical symptoms of vaginal descent, including pelvic pressure, discomfort, urinary incontinence, and visible prolapse requiring medical attention.