Introduction
Rectal prolapse is a painful and uncomfortable condition where part of the rectum slips out of the anal opening. Though it can happen at any age, it is more commonly seen in older adults, women after childbirth, and people with chronic constipation. The good news is that rectal prolapse is treatable and early treatment prevents complications, improves quality of life, and restores normal bowel function.
What Is Rectal Prolapse?
Rectal prolapse occurs when the rectum the last part of the large intestine, slips down from its normal position and protrudes through the anus. This happens due to weak pelvic muscles, nerve damage, or long-term straining during bowel movements.
There are three main types
- Internal Prolapse: The rectum folds inside but does not exit the anus.
- Partial Prolapse: Only the mucosal layer protrudes slightly.
- Complete Prolapse: The entire rectal wall slips out through the anus.
Early diagnosis and proper care can prevent worsening of the prolapse.
Common Causes of Rectal Prolapse
While the exact cause may vary, several risk factors significantly increase the chance of developing rectal prolapse
- Chronic Constipation :- Straining for years weakens the pelvic floor muscles, making prolapse more likely.
- Pregnancy and Childbirth :- Multiple vaginal deliveries or difficult labor may cause pelvic floor weakness.
- Age-Related Muscle Weakness :- Elderly individuals often experience decreased rectal support.
- Nerve Damage :- Conditions like spinal injuries, diabetes, or previous pelvic surgeries can damage nerves that support bowel function.
- Chronic Diarrhea :- Frequent loose stools may also contribute to weakening of the rectal support structures.
Identifying the underlying cause helps doctors recommend a more effective treatment plan.
Symptoms of Rectal Prolapse
Rectal prolapse symptoms may start subtly but often worsen over time. The most common signs include
- A visible bulge from the anus, especially after bowel movements
- Pain, irritation, or itching
- A feeling of incomplete bowel emptying
- Mucus discharge or minor bleeding
- Fecal incontinence, especially in severe prolapse
- Frequent urge to pass stool
If these symptoms are persistent, medical evaluation is essential.
Diagnosis of Rectal Prolapse
Doctors may conduct several exams and tests to confirm the condition
- Physical examination
- Proctoscopy or colonoscopy
- Defecography (X-ray test)
- MRI pelvic scan
- Anal manometry (to check muscle strength)
Accurate diagnosis ensures appropriate treatment and faster recovery.
Best Options for the Treatment of Rectal Prolapse
Treatment depends on the type and severity of the prolapse and the patient’s overall health. Below are the most effective and widely recommended treatments
- Lifestyle and Dietary Changes :- Mild cases may improve with simple modifications
- Increasing fiber intake
- Drinking plenty of water
- Avoiding excessive straining
- Using stool softeners
- Practicing pelvic floor exercises (Kegels)
These methods help control symptoms but are usually not enough for complete prolapse.
- Medications :- Medicines may be prescribed to regulate bowel habits
- Laxatives for constipation
- Antidiarrheal medications for chronic loose stools
- Anti-inflammatory creams for irritation
Medication helps manage symptoms, but cannot correct a full rectal prolapse.
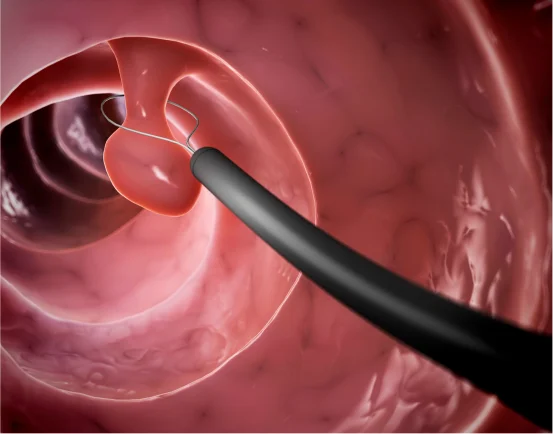
- Minimally Invasive Procedures :- For moderate prolapse, doctors may use minimally invasive surgical options such as
- Laparoscopic rectopexy
- Robotic rectopexy
These procedures involve repositioning the rectum and securing it to the pelvic bones. They offer benefits like
- Small incisions
- Faster recovery
- Less pain
- Lower risk of complications
- Abdominal Surgery for Rectal Prolapse :- This is one of the most effective treatments for full prolapse. The surgeon lifts the rectum and attaches it securely using sutures or mesh. It provides
- Long-term relief
- Improved bowel control
- Very low recurrence rates
This method is preferred in healthy adults.
- Perineal Surgery (Through the Anus) :- This is an option for elderly patients or those with major health conditions. Two main surgery types include
- Altemeier Procedure
- Delorme Procedure
These procedures involve removing the prolapsed tissue and tightening the rectal muscles. They are less invasive but may have a higher recurrence compared to abdominal surgery.
Recovery After Rectal Prolapse Surgery
Most patients experience relief from pain and improved bowel control soon after treatment. Recovery tips include
- Avoid heavy lifting for a few weeks
- Maintain a high-fiber diet
- Take prescribed stool softeners
- Keep the surgical area clean
- Attend follow-up appointments regularly
Proper care ensures long-term success and prevents recurrence.
When to See a Doctor
Consult a specialist immediately if you experience
- Persistent anal bulging
- Difficulty controlling stool
- Bleeding or mucus discharge
- Severe constipation or straining
Early treatment leads to faster recovery and prevents complications.
Conclusion
Rectal prolapse can be distressing, but effective treatments from lifestyle changes to advanced surgical procedures can fully resolve the condition. With proper medical care and timely intervention, patients can return to a normal, comfortable life. If you suspect rectal prolapse or are experiencing symptoms, don’t hesitate to seek medical guidance. Early diagnosis is key to successful treatment and long-term relief.