Introduction
Vaginal descent, commonly referred to as pelvic organ prolapse, is a condition where one or more of the pelvic organs such as the bladder, uterus, or rectum drop from their normal position and push into the vaginal canal. This condition is more common than many realize, affecting millions of women worldwide, especially after childbirth, menopause, or due to chronic strain. Understanding the types of vaginal descent is crucial for early detection, proper management, and maintaining overall pelvic health.
What Is Vaginal Descent?
Vaginal descent occurs when the muscles, ligaments, and tissues that support the pelvic organs weaken, allowing these organs to descend into the vaginal canal. The severity can range from mild, causing minimal discomfort, to severe, where the organ protrudes outside the vaginal opening. While vaginal descent is often associated with aging and childbirth, it can also result from chronic coughing, obesity, heavy lifting, or conditions that increase intra-abdominal pressure.
Common symptoms of vaginal descent include
- A feeling of heaviness or pressure in the pelvic area
- A noticeable bulge or protrusion from the vagina
- Urinary incontinence or difficulty emptying the bladder
- Pain during sexual intercourse
- Lower back pain or discomfort while standing
Early detection and understanding the type of vaginal descent can significantly improve treatment outcomes.
Types of Vaginal Descent
Vaginal descent can be classified based on which organ has prolapsed and its severity. Here are the main types
- Anterior Vaginal Wall Prolapse (Cystocele) :- Anterior vaginal wall prolapse, also known as cystocele, occurs when the bladder descends into the vaginal canal. This happens due to weakening of the tissue between the bladder and the vagina.
Symptoms include
- Frequent urination or urgency
- Difficulty completely emptying the bladder
- Feeling of a bulge at the vaginal opening
Risk factors: Childbirth, aging, obesity, and chronic straining.
- Posterior Vaginal Wall Prolapse (Rectocele) :- Posterior vaginal wall prolapse, or rectocele, occurs when the rectum bulges into the vagina due to weakened tissue at the back of the vaginal wall.
Symptoms include
- Difficulty with bowel movements
- Constipation or straining during defecation
- Feeling of vaginal fullness or bulging
Risk factors: Vaginal delivery, chronic constipation, aging, and connective tissue disorders.
- Uterine Prolapse :- Uterine prolapse happens when the uterus descends into the vaginal canal. Depending on severity, the uterus may remain partially inside or protrude outside the vaginal opening.
Symptoms include
- Sensation of heaviness in the pelvis
- Vaginal bulge or tissue protrusion
- Pain during intercourse
- Urinary or bowel problems
Risk factors: Multiple vaginal deliveries, weakened pelvic muscles, menopause, and chronic straining.
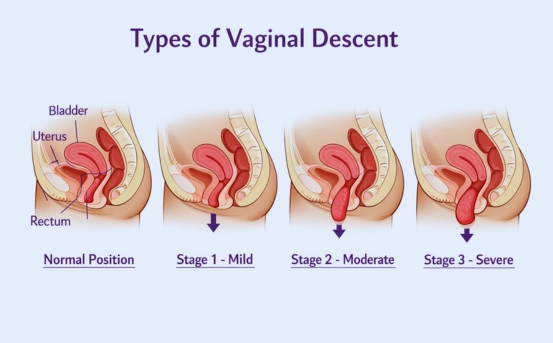
Uterine prolapse is often graded in stages
- Stage 1: Mild descent; uterus remains inside the vagina
- Stage 2: Moderate descent; uterus reaches the vaginal opening
- Stage 3: Severe descent; uterus protrudes outside the vagina
- Stage 4: Complete prolapse; uterus fully outside the vaginal canal
- Enterocele :- Enterocele is a type of vaginal prolapse where the small intestine descends into the upper part of the vaginal canal, often occurring after a hysterectomy.
Symptoms include
- Lower abdominal or pelvic pressure
- Vaginal bulging
- Discomfort while standing or lifting
Risk factors: Previous pelvic surgery, aging, or weakened pelvic floor muscles.
- Combined or Multi-Compartment Prolapse :- In some cases, more than one pelvic organ may prolapse simultaneously, leading to a combination of cystocele, rectocele, and uterine prolapse. This multi-compartment prolapse can be more complex to treat and may require surgical intervention.
Symptoms include
- Severe pelvic pressure and discomfort
- Urinary and bowel dysfunction
- Difficulty with daily activities
Causes of Vaginal Descent
Vaginal descent generally occurs due to a combination of factors that weaken the pelvic support system
- Childbirth: Vaginal delivery, especially with large babies or multiple births, can stretch and weaken pelvic muscles.
- Aging and Menopause: Decreased estrogen levels reduce tissue elasticity and strength.
- Chronic Strain: Persistent coughing, constipation, or heavy lifting increases pressure on pelvic organs.
- Genetics: Some women have naturally weaker connective tissue, making them more susceptible.
- Obesity: Excess weight increases pressure on the pelvic floor.
Diagnosis
A gynecologist or pelvic health specialist can diagnose vaginal descent through
- Physical pelvic examination
- Imaging studies like ultrasound or MRI in complex cases
- Urodynamic tests to assess bladder function
Treatment Options
The treatment for vaginal descent depends on the type, severity, and symptoms. Common approaches include
- Lifestyle Modifications: Weight management, avoiding heavy lifting, and treating chronic constipation.
- Pelvic Floor Exercises: Kegel exercises strengthen pelvic muscles and improve support.
- Pessary Devices: A removable device inserted into the vagina to support prolapsed organs.
- Hormonal Therapy: Vaginal estrogen creams may improve tissue strength in postmenopausal women.
- Surgical Intervention: In severe cases, surgery may be required to repair prolapsed organs or restore normal anatomy.
Prevention
While vaginal descent cannot always be prevented, certain measures can reduce risk
- Regular pelvic floor exercises
- Maintaining a healthy weight
- Avoiding chronic straining
- Seeking early medical advice after childbirth or pelvic injury
Conclusion
Understanding the types of vaginal descent is vital for recognizing early symptoms and seeking timely treatment. From cystocele and rectocele to uterine prolapse and enterocele, each type presents unique challenges but can be managed effectively with the right approach. Consulting a specialist, performing pelvic floor exercises, and adopting preventive measures can help women maintain pelvic health and improve quality of life.