Introduction
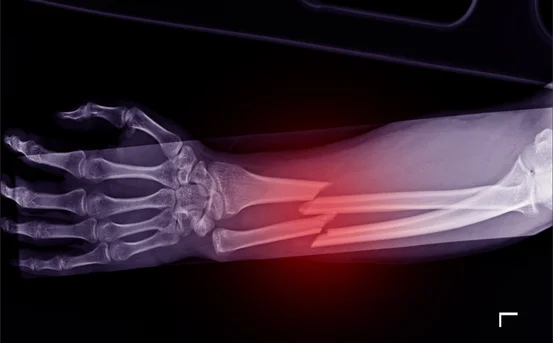
Fracture repair is an important biological process that helps restore the bone’s integrity after a fracture. The process involves a complicated interaction of cellular processes biochemical pathways, as well as mechanical elements that work to repair the fractured bone. Fractures can result from injury or overuse, as well as diseases such as osteoporosis. The healing process generally follows a set of well-defined phases, and could require medical attention based on the severity and location the fracture.
Types of Fractures
Fractures are classified into various kinds based on the characteristics of their respective:
- Easy (Closed) Broken bone :- The bone is broken but doesn’t penetrate into the skin.
- Compound (Open) Fracture :- The fractured bone penetrates the skin, thereby increasing the risk of infection.
- Comminuted Fracture :- The bone breaks into several pieces.
- Greenstick Fracture :- A partial break in which the bone bends and cracks. This is common in children.
- Transverse Fracture :- A fracture that is formed in an uniform line across the bone.
- Oblique Fracture :- A break diagonally along the bony structure.
- Spiral Fracture :- A split caused by twisting force.
- A pathological fracture :- It is a fracture that occurs from weak bones caused by the disease.
- stress fracture :- A small fracture in the bone resulting from repeated stress or excessive use.
Phases of Fracture Healing
Repairing a fracture can occur in four main phases:
1. Inflammatory Phase (Hematoma Formation) :- After an injury there is a blood vessel rupture within the bone break and lead to formation of the hemoglobin (blood clot) at the site of injury. The hematoma acts as a platform for the growth of new cells that can begin the process of healing. Inflammatory cells, such as neutrophils and macrophages infiltrate the area, and release growth factors and cytokines to are able to attract bone-forming cells.
2. Fibrocartilaginous (Soft) Callus Formation :- Within a couple of days to weeks the chondroblasts and fibroblasts invade the hematoma and form an elongated callus made of cartilage and collagen. This temporary structure bridges broken bone’s edges and stabilizes the bone for continued healing.
3. Bony (Hard) Callus Formation :- In the coming weeks osteoblasts will are able to replace soft callsus by the hard bone callus that is mineralized. Calcium and phosphate are released to strengthen bone. The new callus is more structurally strong, but not as strong as the bone that was originally.
4. Bone Remodeling :- The healing process could last from months or even years. Osteoclasts remove bone tissue, and reshape the newly formed bone in order to rebuild its original structure and strength. Bone development is influenced by mechanical stress and regular usage of the limb assists in the final process of strengthening.
Factors Affecting Fracture Healing
A variety of factors affect the rate and effectiveness of repair for fractures:
- Age :- Younger people are healthier due to greater cells’ activity and an improved blood supply.
- Blood Supply :- An adequate flow of blood ensures the proper flow of nutrients and oxygen, which are vital for healing.
- the type and location :- Simple fractures heal quicker than fractures that are complex or comminuted.
- Infection :- Fractures that are open are more prone to infection, which could cause delays in healing.
- medical conditions :- Conditions such as osteoporosis, diabetes, and vascular diseases can affect healing.
- Lifestyle Factors :- Smoking, poor nutrition and drinking excessively can negatively affect the repair of bone.
Medical Interventions for Fracture Repair
Based on the extent of the fracture various methods can be utilized to aid healing:
1. Immobilization :- In the case of small fractures, immobilization with casts, splints or braces can help maintain the bone’s position which allows healing to occur naturally.
2. Closed Reduction :- In the event that bone’s ends become not aligned A healthcare professional may manually align them, without surgery. This is followed by immobilization.
3. Open Reduction and Internal Fixation (ORIF) :- In severe fractures, it is common to require surgical treatment, in which screws, metal plates or rods are utilized to support the bone.
4. External Fixation :- In more severe fractures the frame externally connected to the bone using pins that are inserted into the skin, to keep the bone securely while it heals.
5. Bone Grafting :- In the case of fractures that have large bone losses, the grafting procedure can be carried out to encourage the growth of bone.
6. Physical Therapy :- Following initial recovery, exercises to can help to restore mobility, strength and functionality to the afflicted leg.
Complications of Fracture Healing
Although most fractures heal without problems but complications can occur:
- Delayed union :- The healing process for the fracture occurs slower than anticipated.
- Nonunion :- The bone does not heal which requires further treatment.
- Malunion :- The bone heals incorrectly in a place, which causes deformity.
- Infection :- Most common for open-fracture fractures. Infections may hinder healing and may require surgery or antibiotics.
- Avascular necrosis :- The loss of blood supply to bone could cause bone loss and may require surgery.
- Compartment Syndrome :- An increase in pressure inside the muscle compartment could cause serious damage and require urgent treatment.
Conclusion
Repairing fractures is a complicated but extremely coordinated procedure that helps bones restore its strength as well as function following injuries. The healing process is governed by specific biological phases, which are affected by a variety of aspects like age, blood supply and medical ailments. Although most fractures heal using conventional treatments, a few require surgery to ensure align and stabilization. Understanding the fundamentals of repairing fractures is helpful in optimizing treatment strategies as well as improving the outcomes of patients.