Introduction
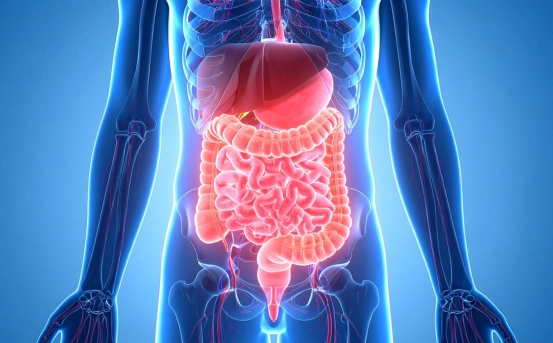
Mesenteric ischemia is a serious medical condition that occurs when there is insufficient blood flow to the intestines, leading to reduced oxygen and nutrient supply to the bowel tissues. The term “mesenteric” refers to the mesentery, a network of blood vessels that supplies the small and large intestines, while “ischemia” means a lack of adequate blood flow. When this circulation is compromised, the intestinal tissues can become damaged or even die if treatment is delayed. Mesenteric ischemia can develop suddenly or progress gradually over time. Because the intestines play a vital role in digestion and nutrient absorption, this condition can quickly become life-threatening. Early recognition and prompt medical intervention are essential to prevent severe complications.
Understanding What is Mesenteric Ischemia
The intestines receive blood through three major arteries branching from the abdominal aorta
- Superior Mesenteric Artery (SMA) supplies most of the small intestine and part of the large intestine
- Inferior Mesenteric Artery (IMA) supplies the lower portion of the large intestine
- Celiac Artery supplies the stomach, liver, and upper digestive organs
Any blockage, narrowing, or spasm in these vessels can disrupt blood flow and lead to mesenteric ischemia. When the intestinal tissues are deprived of oxygen, inflammation, tissue injury, and necrosis (tissue death) may occur.
Types of Mesenteric Ischemia
Mesenteric ischemia is classified into different types based on its onset and cause
- Acute Mesenteric Ischemia :- This is a sudden and severe form of the condition and is considered a medical emergency. It typically results from
- A blood clot blocking a mesenteric artery
- An embolus (a clot that travels from the heart)
- Sudden narrowing of blood vessels due to shock or low blood pressure
Acute mesenteric ischemia can cause rapid intestinal damage and requires immediate treatment to save the bowel and the patient’s life.
- Chronic Mesenteric Ischemia :- This form develops gradually over time, usually due to progressive narrowing of the mesenteric arteries caused by atherosclerosis (plaque buildup). Patients may experience recurring symptoms after meals, as digestion increases the intestine’s demand for blood.
- Non-Occlusive Mesenteric Ischemia :- In this type, there is no physical blockage in the artery. Instead, reduced blood flow occurs due to
- Severe heart failure
- Shock
- Low blood pressure
- Certain medications that constrict blood vessels
- Mesenteric Venous Thrombosis :- This occurs when a blood clot forms in the mesenteric veins, preventing blood from draining out of the intestines. As pressure builds up, circulation is impaired, leading to intestinal swelling and injury.
Causes of Mesenteric Ischemia
Several factors can contribute to the development of mesenteric ischemia, including
- Atherosclerosis (hardening of the arteries)
- Blood clots or emboli
- Heart rhythm disorders such as atrial fibrillation
- Low blood pressure or shock
- Severe dehydration
- Blood clotting disorders
- Smoking
- Advanced age
- History of cardiovascular disease
Chronic mesenteric ischemia is most commonly linked to long-term vascular disease, while acute cases are often caused by sudden arterial blockage.
Symptoms of Mesenteric Ischemia
The symptoms vary depending on the type and severity of the condition
- Acute Mesenteric Ischemia Symptoms
- Sudden, severe abdominal pain
- Pain disproportionate to physical findings
- Nausea and vomiting
- Diarrhea or bloody stools
- Abdominal distension
- Fever and rapid heart rate
- Chronic Mesenteric Ischemia Symptoms
- Abdominal pain after eating
- Fear of eating due to pain
- Unintentional weight loss
- Bloating or diarrhea
- Fatigue
Because early symptoms can be vague, mesenteric ischemia is sometimes misdiagnosed, leading to dangerous delays in treatment.
Diagnosis of Mesenteric Ischemia
Accurate and rapid diagnosis is crucial. Doctors may use several diagnostic tools, including
- CT angiography the most effective imaging method to assess blood flow in mesenteric vessels
- Doppler ultrasound to evaluate arterial blood flow
- Blood tests to check for infection, metabolic abnormalities, or elevated lactate levels
- Conventional angiography allows direct visualization of blood vessels and potential treatment
Early imaging significantly improves outcomes by enabling prompt intervention.
Treatment Overview
The treatment of mesenteric ischemia depends on its type and severity
- Acute mesenteric ischemia often requires emergency surgery to remove blood clots, restore circulation, or remove damaged bowel segments.
- Chronic mesenteric ischemia is usually treated with procedures to restore blood flow, such as angioplasty, stenting, or bypass surgery.
- Non-occlusive ischemia focuses on stabilizing blood pressure and improving circulation.
- Mesenteric venous thrombosis is typically treated with anticoagulant medications.
Early treatment can prevent bowel death, sepsis, and multi-organ failure.
Complications of Untreated Mesenteric Ischemia
If left untreated, mesenteric ischemia can lead to serious complications such as
- Intestinal necrosis
- Bowel perforation
- Severe infection (sepsis)
- Short bowel syndrome
- Organ failure
- Death
These complications highlight the importance of early recognition and timely medical care.
Conclusion
Mesenteric ischemia is a potentially life-threatening condition caused by reduced blood flow to the intestines. It can present suddenly or develop gradually, depending on the underlying cause. While symptoms may initially be subtle, delayed diagnosis can result in severe intestinal damage and fatal complications. Understanding the causes, types, and warning signs of mesenteric ischemia is essential for early detection and effective treatment. Advances in imaging, surgical techniques, and endovascular therapies have significantly improved patient outcomes. However, prompt medical attention remains the most critical factor in saving both intestinal function and life.