Introduction
Vaginal descent, also known as vaginal prolapse or pelvic organ prolapse, is a condition where the vaginal walls or surrounding pelvic organs descend from their normal position. This condition mainly affects women, particularly those who have given birth, and can significantly impact daily life and overall quality of life if left untreated. Understanding the causes, symptoms, and treatment options is crucial for early detection and effective management.
Understanding What is Vaginal Descent
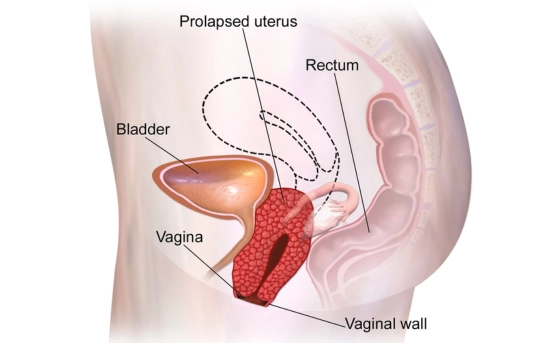
Vaginal descent occurs when the muscles, ligaments, and tissues that support the pelvic organs weaken. These pelvic organs include the bladder, uterus, rectum, and small intestines. When these structures lose their support, they can push against the vaginal walls, causing a bulge or protrusion. Vaginal descent is classified into different types depending on which organ is affected
- Cystocele: When the bladder descends into the front wall of the vagina.
- Rectocele: When the rectum bulges into the back wall of the vagina.
- Uterine Prolapse: When the uterus descends into the vaginal canal.
- Enterocele: When the small intestine pushes into the vagina.
The severity of vaginal descent can vary from mild to severe, ranging from slight discomfort to a noticeable protrusion outside the vaginal opening.
Causes of Vaginal Descent
Several factors can contribute to vaginal descent, including
- Childbirth: Vaginal delivery, especially multiple deliveries or delivery of large babies, can weaken pelvic floor muscles.
- Aging: As women age, hormonal changes during menopause, particularly decreased estrogen levels, can reduce tissue elasticity.
- Obesity: Excess body weight increases pressure on the pelvic floor, leading to muscle weakening.
- Chronic Cough or Constipation: Repeated straining can put additional stress on pelvic structures.
- Previous Pelvic Surgery: Surgeries like hysterectomy may sometimes weaken support structures, increasing the risk.
- Genetic Factors: Some women have naturally weaker connective tissues, making them more prone to prolapse.
Symptoms of Vaginal Descent
The symptoms of vaginal descent vary depending on the type and severity of the prolapse. Common symptoms include
- Feeling of pressure or heaviness in the pelvic area
- A bulge or protrusion at the vaginal opening
- Discomfort during sexual intercourse
- Lower back pain
- Urinary problems such as leakage, frequent urination, or difficulty emptying the bladder
- Bowel issues, including constipation or difficulty controlling bowel movements
- Recurrent urinary tract infections
Mild cases may remain unnoticed, while severe prolapse can interfere with daily activities and significantly affect quality of life.
Diagnosing Vaginal Descent
Diagnosis usually involves a detailed medical history, physical examination, and sometimes imaging tests. A gynecologist may perform a pelvic examination to assess the degree of prolapse and identify which pelvic organs are involved. Imaging techniques like ultrasound, MRI, or defecography may be recommended for complex cases to evaluate the extent of descent and plan treatment.
Treatment Options for Vaginal Descent
Treatment for vaginal descent depends on the severity of the condition, the patient’s symptoms, age, and overall health. Options include conservative management and surgical intervention.
- Conservative Treatments :- For mild cases of vaginal descent, non-surgical options may help relieve symptoms:
- Pelvic Floor Exercises: Also known as Kegel exercises, these strengthen the pelvic muscles and improve support.
- Lifestyle Modifications: Weight loss, avoiding heavy lifting, and treating chronic cough or constipation can reduce strain on the pelvic floor.
- Pessary Devices: A vaginal pessary is a removable device inserted into the vagina to support the pelvic organs and relieve symptoms.
- Surgical Treatments :- When conservative measures fail or prolapse is severe, surgery may be recommended. Surgical options include
- Vaginal or Abdominal Repair: Reconstructive surgery strengthens the weakened pelvic tissues and restores organs to their normal position.
- Hysterectomy: In cases of severe uterine prolapse, removal of the uterus may be considered.
- Mesh Repair: In certain situations, surgical mesh is used to support the pelvic floor, though its use is carefully evaluated due to potential complications.
The choice of procedure is individualized and discussed thoroughly with the gynecologist to achieve the best outcomes.
Prevention of Vaginal Descent
While not all cases of vaginal descent can be prevented, certain measures may reduce the risk
- Performing regular pelvic floor exercises
- Maintaining a healthy body weight
- Avoiding chronic straining during bowel movements
- Practicing proper lifting techniques
- Seeking prompt treatment for chronic cough or respiratory issues
- Managing hormonal changes with medical guidance
Early intervention can prevent the condition from worsening and improve quality of life.
When to See a Doctor
If you experience symptoms such as pelvic pressure, bulging, urinary or bowel issues, or pain during intercourse, it’s important to consult a gynecologist. Early diagnosis and treatment can prevent complications and provide effective relief.
Conclusion
Vaginal descent is a common condition affecting many women, especially after childbirth or during aging. Recognizing the symptoms early, seeking timely medical care, and adopting preventive measures can make a significant difference. With advancements in conservative and surgical treatments, women can regain comfort, confidence, and normal daily function.