Introduction
Acute Limb Ischemia (ALI) is a serious medical emergency characterized by a sudden decrease in blood flow to a limb, most commonly the legs, which can threaten limb viability if not treated promptly. Early recognition and intervention are crucial to prevent permanent tissue damage or even amputation. Understanding the types of acute limb ischemia, their causes, and associated risk factors can help patients and healthcare providers respond effectively.
What is Acute Limb Ischemia?
Acute Limb Ischemia occurs when an artery supplying blood to a limb is suddenly blocked, reducing oxygen and nutrient supply. The condition is different from chronic peripheral artery disease, which develops gradually over time. ALI usually presents with the classic “6 Ps”: Pain, Pallor, Pulselessness, Paresthesia, Paralysis, and Poikilothermia (cold limb). These symptoms require urgent attention, as the affected tissue may start dying within hours. The incidence of ALI is estimated at 1.5 cases per 10,000 people annually, with higher risk among individuals with cardiovascular disease, diabetes, or a history of blood clots.
Causes of Acute Limb Ischemia
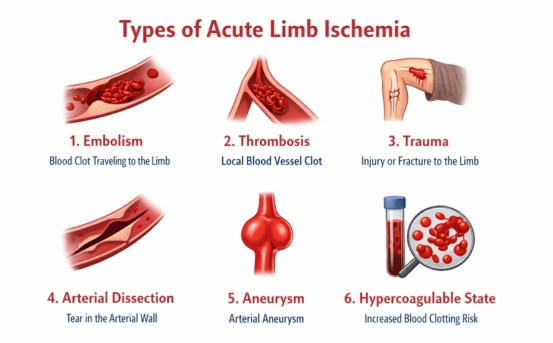
The causes of acute limb ischemia typically fall into three main categories
- Embolism: A blood clot or other material travels from another part of the body, often the heart, and lodges in a peripheral artery. Embolic events are frequently seen in patients with atrial fibrillation, heart valve disease, or after heart surgery.
- Thrombosis: A clot forms directly in a diseased artery, often one already narrowed by atherosclerosis. Thrombosis can occur spontaneously or be triggered by trauma, surgery, or severe infection.
- Trauma or Arterial Injury: Physical injury, such as fractures or vascular surgery, can cause sudden arterial blockage leading to ischemia.
- Other Rare Causes: Conditions like arterial dissection, hypercoagulable states, or severe vasospasm may also trigger acute limb ischemia.
Types of Acute Limb Ischemia
Acute Limb Ischemia can be categorized based on severity, onset, and the underlying cause. Knowing the type helps determine the urgency and type of treatment.
- Embolic Acute Limb Ischemia :- Embolic ALI occurs when a clot or debris travels from a distant site, usually the heart, and obstructs a peripheral artery. It accounts for approximately 40% of acute limb ischemia cases.
Key Features
- Sudden onset of symptoms
- Severe pain in the affected limb
- No prior history of claudication (leg pain during walking)
- Limb appears pale and cool
- Weak or absent pulse in the affected artery
Common Causes
- Atrial fibrillation
- Myocardial infarction with mural thrombus
- Endocarditis
- Artificial heart valves
Treatment :- Embolic ALI often requires urgent surgical embolectomy or catheter-directed thrombolysis to remove the clot and restore blood flow.
- Thrombotic Acute Limb Ischemia :- Thrombotic ALI occurs when a blood clot forms within a diseased artery, usually affected by chronic atherosclerosis. Unlike embolic ALI, thrombotic events may develop more gradually, sometimes giving warning signs such as intermittent claudication.
Key Features
- Limb pain may develop over hours or days
- History of peripheral artery disease
- Reduced or absent pulse distal to the blockage
- Skin may appear mottled or cyanotic
Common Causes
- Advanced atherosclerosis
- Hypercoagulable disorders
- Previous stent or graft occlusion
Treatment :- Thrombotic ALI is managed with a combination of anticoagulants, thrombolytic therapy, or surgical bypass, depending on the location and severity of the blockage.
- Iatrogenic Acute Limb Ischemia :- Iatrogenic ALI is caused by medical procedures or interventions, such as arterial catheterization, vascular surgery, or stent placement. Although less common, it is an important consideration in post-surgical patients.
Key Features
- Occurs shortly after an invasive procedure
- Localized pain and swelling
- Signs of reduced blood flow (cold limb, weak pulse)
Treatment :- Immediate intervention involves removing the obstruction, often via angioplasty, stenting, or surgical correction, combined with anticoagulation therapy.
- Traumatic Acute Limb Ischemia :- Trauma-induced ALI occurs when direct injury to an artery obstructs blood flow. It may result from fractures, crush injuries, or penetrating trauma.
Key Features
- History of trauma
- Rapid onset of severe pain
- Cold, pale, or blue limb
- Loss of sensation or movement
Treatment :- Traumatic ALI often requires surgical repair of the artery, along with fracture stabilization if necessary, and supportive care to restore circulation.
Classification by Severity
In addition to the cause, ALI is classified by severity, which guides treatment decisions
- Viable Limb (Category I): Limb is not immediately threatened; pulses may be diminished, but there is no sensory loss or motor deficit. Urgent medical management is required.
- Threatened Limb (Category IIa and IIb): Limb shows sensory loss, mild to moderate motor impairment, and diminished perfusion. Immediate revascularization is necessary.
- Irreversible Limb (Category III): Extensive tissue damage is present; limb may be cold, anesthetic, and paralyzed. Amputation is often required.
Risk Factors for Acute Limb Ischemia
Several factors increase the likelihood of ALI
- Peripheral artery disease
- Atrial fibrillation
- Heart valve disease
- Diabetes mellitus
- Smoking
- Recent surgery or trauma
- Hypercoagulable states
Diagnosis of Acute Limb Ischemia
Early diagnosis is crucial for saving the limb. Diagnostic approaches include
- Physical examination: Checking pulses, skin color, temperature, and sensation
- Doppler ultrasound: Evaluates blood flow
- CT Angiography (CTA) or MR Angiography (MRA): Identifies site and cause of obstruction
- Blood tests: Assess clotting profile and tissue damage markers
Treatment and Management
Management depends on the type and severity of ALI
- Anticoagulation: Heparin is typically administered to prevent further clot formation.
- Thrombolysis: Catheter-directed clot-dissolving medications may restore blood flow.
- Surgery: Embolectomy, bypass grafting, or arterial repair may be needed in severe cases.
- Supportive care: Pain management, wound care, and rehabilitation are essential after revascularization.
Prompt treatment within 6 hours significantly increases the chance of limb salvage.
Conclusion
Acute Limb Ischemia is a medical emergency that requires rapid recognition and intervention. Understanding the types of acute limb ischemia embolic, thrombotic, iatrogenic, and traumatic helps in early diagnosis and timely treatment, preventing irreversible limb damage. If you or someone experiences sudden limb pain, pallor, or loss of pulse, seek immediate medical attention to save the limb and prevent complications.