Introduction
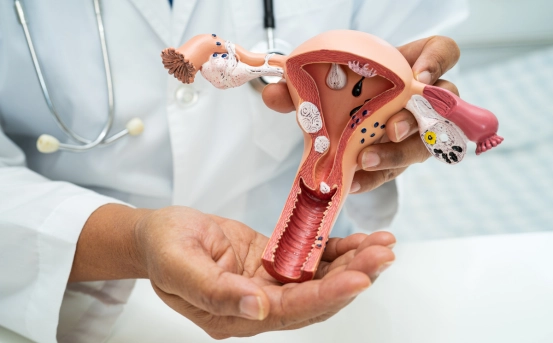
Hysteroscopy is a specialized medical procedure that allows doctors to examine the inside of a woman’s uterus using a thin, lighted instrument called a hysteroscope. This minimally invasive procedure has transformed gynecology, offering a precise way to diagnose and treat uterine problems without the need for major surgery. Hysteroscopy is widely used for both diagnostic and therapeutic purposes, making it a vital tool for women’s reproductive health.
What is Hysteroscopy?
Hysteroscopy is a minimally invasive procedure that enables direct visualization of the uterine cavity. Using a hysteroscope a thin tube equipped with a light and camera gynecologists can examine the uterus for abnormalities such as polyps, fibroids, adhesions, or congenital malformations. Unlike traditional methods like dilation and curettage (D&C), hysteroscopy provides real-time imaging, allowing for accurate diagnosis and immediate treatment if necessary. The procedure can be performed in a hospital or outpatient setting, often under local or general anesthesia, depending on the complexity of the treatment. Hysteroscopy has become increasingly popular because it reduces recovery time, minimizes complications, and provides a clearer view of uterine structures compared to other methods.
Why is Hysteroscopy Performed?
Hysteroscopy is commonly recommended for women experiencing:
- Abnormal uterine bleeding: Unexplained heavy, prolonged, or irregular menstrual bleeding.
- Infertility: To check for uterine issues that may affect conception or implantation.
- Recurrent miscarriages: Detecting structural abnormalities or scar tissue.
- Suspected uterine growths: Polyps, fibroids, or tumors inside the uterine cavity.
- Endometrial sampling: To evaluate abnormal endometrial tissue or rule out cancer.
By providing a direct view of the uterus, hysteroscopy allows for accurate diagnosis, which is essential for effective treatment planning.
Types of Hysteroscopy
Hysteroscopy can be classified into two main types:
- Diagnostic Hysteroscopy :-This is performed primarily to inspect the uterine cavity. A thin hysteroscope is inserted to detect abnormalities like polyps, fibroids, adhesions, or congenital malformations. It usually doesn’t involve major surgical procedures and is often done as an outpatient procedure.
- Operative Hysteroscopy :- Operative hysteroscopy is used to treat identified problems during the same procedure. Instruments can be passed through the hysteroscope to remove polyps, fibroids, adhesions, or septa. This type reduces the need for multiple procedures and accelerates recovery.
The Hysteroscopy Procedure
The hysteroscopy procedure is generally straightforward and safe. Here’s what to expect:
- Preparation:
- The doctor may recommend avoiding food or drink for a few hours before the procedure if general anesthesia is used.
- Certain medications or pre-procedure exams may be required.
- During the Procedure:
- The patient lies on an examination table, similar to a routine gynecological exam.
- A speculum is inserted to access the cervix, and the hysteroscope is gently introduced into the uterus.
- Saline or carbon dioxide may be used to expand the uterus for better visibility.
- The doctor examines the uterine cavity and may perform treatments like polyp removal, fibroid resection, or biopsy.
- Duration:
- Diagnostic hysteroscopy typically lasts 5–15 minutes.
- Operative hysteroscopy may take 30–60 minutes, depending on the complexity.
- Post-Procedure:
- Patients may experience mild cramping, spotting, or discharge for a few days.
- Most can resume normal activities within a day or two.
Benefits of Hysteroscopy
Hysteroscopy offers numerous advantages compared to traditional methods:
- Minimally invasive: No large incisions are needed, reducing pain and scarring.
- Accurate diagnosis: Provides real-time imaging for precise identification of uterine issues.
- Combined diagnosis and treatment: Operative hysteroscopy allows immediate treatment during the same session.
- Faster recovery: Most patients resume daily activities within a few days.
- Lower risk of complications: Compared to open surgery, hysteroscopy carries minimal risks.
Risks and Complications
Although hysteroscopy is generally safe, like all medical procedures, it carries some risks:
- Infection: Rare but possible; antibiotics may be prescribed if necessary.
- Uterine perforation: Occurs in less than 1% of cases; usually heals without surgery.
- Bleeding: Minor bleeding is common post-procedure.
- Adhesions: Rarely, scar tissue may form inside the uterus after surgery.
Patients are advised to discuss their medical history and any concerns with their gynecologist before undergoing hysteroscopy.
Recovery and Aftercare
Recovery from hysteroscopy is typically quick:
- Mild discomfort: Cramping or light bleeding may occur for a few days.
- Activity: Most women can return to work and normal activities within 24–48 hours.
- Follow-up: A follow-up visit may be scheduled to review results or ensure proper healing.
- Precautions: Avoid heavy lifting, sexual intercourse, or use of tampons for a short period as advised by your doctor.
Maintaining proper hygiene and following the doctor’s instructions significantly enhances recovery and reduces complications.
Conclusion
Hysteroscopy has revolutionized gynecological care by offering a minimally invasive, highly effective method for diagnosing and treating uterine problems. Whether it is abnormal bleeding, infertility, or uterine growths, hysteroscopy provides precise insight and treatment, often in a single visit. With its high success rates, minimal risks, and quick recovery, hysteroscopy has become an essential tool for modern women’s health.
If you are experiencing unexplained menstrual issues, fertility challenges, or recurrent miscarriages, consulting a gynecologist about hysteroscopy could be a significant step towards understanding and addressing the underlying causes.